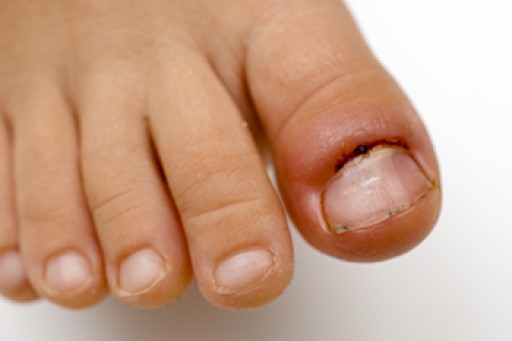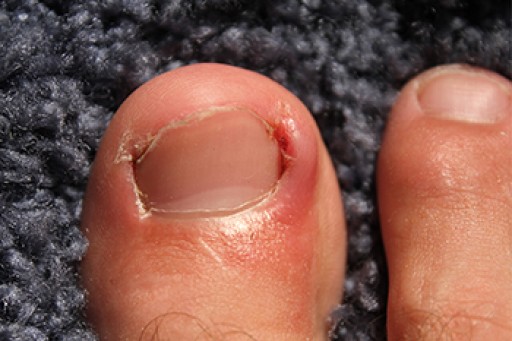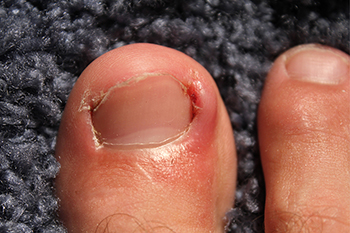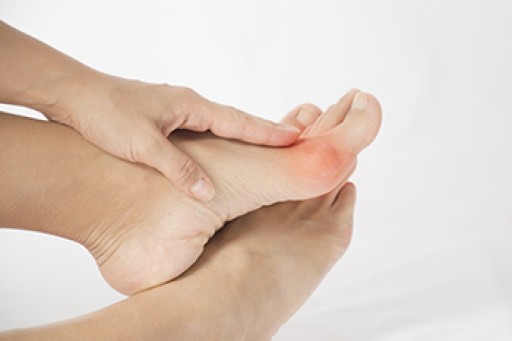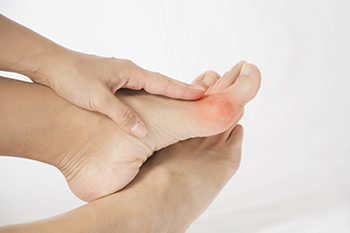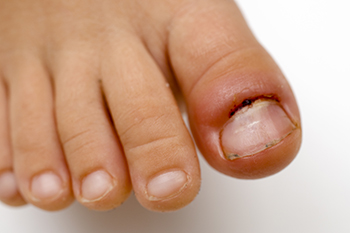
Our toes, those often overlooked companions on our daily journeys, play a more significant role in our lives than we realize, until they ache. Toe pain, a distressing sensation that can impede our daily activities, can arise from various sources. Wearing uncomfortable footwear, such as tight or ill-fitting shoes, may lead to blisters and calluses caused by excess friction. Stubbing a toe, seemingly harmless but potent in its impact, can result in acute pain and potential fractures. Ingrown toenails, a product of improper trimming or wearing shoes that do not fit correctly, can also trigger sharp, localized pain. Athlete's foot, a fungal infection, often targets the spaces between our toes, bringing about itchiness and discomfort. Arthritis can also affect the toes, leading to persistent toe pain. Acknowledging these common culprits empowers us to take better care of our toes, ensuring they continue to walk us through life's adventures without unnecessary pain. If you are experiencing toe pain, it is suggested that you confer with a podiatrist for proper treatment.
Toe pain can disrupt your daily activities. If you have any concerns, contact Cary Golub, DPM of New York. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please feel free to contact our offices located in Williston Park, and Long Beach, NY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.